Chalazion
Meibomian (“my-boh-mee-an”) glands are 20-40 toothpaste tube (slightly crooked though) shaped glands, lined along eye lashes in our eye lids which secrete the oil layer of our tear film to prevent evaporation of our tears too quickly by creating surface tension (making a film of water stay vertical despite gravity).

Blockage, disease or inflammation of these glands results in Meibomian Gland Dysfunction (MGD). Imagine now that when one or multiple of these meibomian glands are blocked that their secretions (meibum) stagnates in the gland forming a cyst-like lesion known as chalazion (external hordeolum). This is differentiated from a stye (internal hordeolum) which usually represents an infection and is more painful and inflamed.
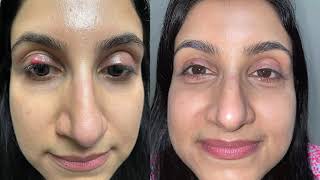
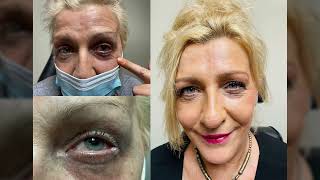
A chalazion therefore presents itself as a bump on the eyelid which in most cases is not painful or inflamed but could present with symptoms ranging from swollen eyelid, to irritation, to even blurry vision in advanced cases.

Primary Treatment:
The age-old treatment of chalazion is to begin with conservative management using warm compresses and steroid based medications which may need surgical I&D (incision and drainage) as a definitive treatment for recalcitrant cases.
Meibomian Gland Recanalization:
Dr. Gulani has been using Meibomian Gland Recanalization (MGR), as a modified meibomian gland probing (MGP) wherein differential probing is performed to the endpoint of recanalization as evidenced by release of trapped meibum and insertion of the marked probe. This technique has successfully treated MGD based dry eyes to the point of even converting them into candidates for laser vision and premium cataract surgery.

Meibomian gland recanalization involves application of reusable and disposable differential probes to cannulate the meibomian gland ducts thereby removing the obstruction and facilitating the release of meibum. The procedure is done in office under topical anesthesia with no injections or needles. Numbing is achieved with a specially formulated gel that is directly applied to the eyelid skin. A dedicated attempt is made to open each and every gland, followed by mechanical compression using specially designed atraumatic forceps to release the initial stagnant and mostly cheesy meibum. This procedure, which may take anywhere from 10 to 15 minutes, is then followed by a proprietary medication and ocular hygiene protocol.
Surgical Removal:
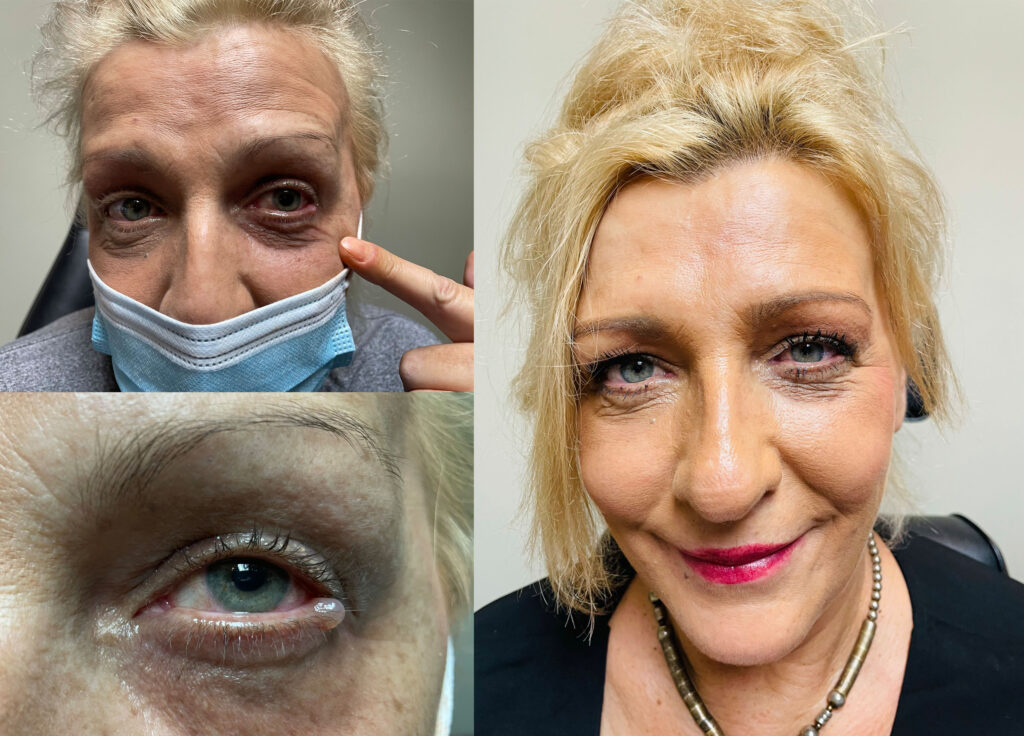
Having had consistent success with Dr. Gulani’s proprietary m.o.i.s.t.® therapy which includes meibomian gland recanalization for chalazion, Dr. Gulani was inspired to develop and apply a “No-Incision Chalazion Expression” (NICETM) technique for recalcitrant chalazia with gratifying results both, objectively and subjectively. This least interventional and elegant approach is in contrast with the more invasive Incision and Drainage (I&D) surgery approach (where injected anesthesia is needed, along with possibility of scarring, and high chance of recurrence). Patients from around the world have benefited from this NICETM technique which takes 10-15 minutes the difficulty level of this technique calls for Dr. Gulani’s over 3 decades of artistic skills to selectively find the blocked glands and release the stagnant meibum. This is in contrast to I&D, where a blade is taken across the affected area, and adversely impacts the anatomy and function of the glands in the future.
Correcting Failed Therapy:
As a world resource for dry eye correction, Dr. Gulani is often called upon by colleagues as well as sought by patients for second opinion for failed treatments for chalazion. Failure by previous surgeons could be caused by inability to remove the entire chalazion, surgical complication, or recurrence. These previous treatment modalities could be from Lipiflow, IPL, Blephex, iLux, TearCare, including surgical I&D. Using his proprietary differential recanalization approach (NICETM) Dr. Gulani has successfully reversed and corrected many such surgically failed and complicated patients from all over the world.